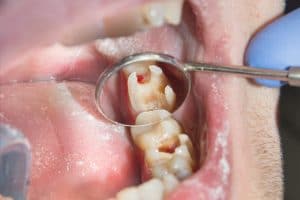
How To Know If You Need A Root Canal
The Purpose of Sedation Dentistry
March 15, 2019How To Whiten Your Smile
April 5, 2019
Root canals provide patients with an alternative to tooth extraction when infection has compromised the strength of a tooth. A root canal has multiple meanings, but typically refers to the actual passage within the tooth between the pulp and tooth roots that contain nerves and blood vessels. When this area gets infected, a root canal procedure is needed to clean out the infected tooth pulp. Learn how to recognize whether you need a root canal and what the process entails through this guide!
What Is A Root Canal?
A very common dental procedure that many patients will receive during their lifetime is a root canal. When infection and decay have compromised the integrity of a tooth’s pulp, root canals are common procedures to fix the infection without having to pull the tooth. Root canal therapy removes damaged tissue from the inside of your teeth and disinfects the canal of the affected tooth. Our teeth are meant to last us for a lifetime, so root canal therapy can help us avoid getting teeth pulled from disease or injury. Root canal has a few definitions, but it mainly refers to the actual passages within the tooth between the pulp and the tooth roots that contain blood vessels and nerves. When the pulp of the tooth becomes infected, your dentist will remove the nerve and infected pulp inside the tooth to eliminate the infection. This type of tooth infection can be very painful, and cannot be fixed by simply ignoring it or taking pain medication. If not treated, the tissues around the tooth can become infected, and you can lose the tooth entirely. According to the American Association of Endodontists, more than 15 million root canals are performed each year; that’s 41,000 root canals each day, so it’s a common treatment. Meeting with your dentist for an examination early on when experiencing any tooth pain can be a matter of saving or losing your tooth. Knowing what signs to look out for and how to recognize whether your toothache is something more severe are some of the first steps in safeguarding the health of your teeth.
Signs You Need A Root Canal
An infected root canal can be caused by one of three things: decay, disease, or damage. When tooth decay penetrates the outer layer of a tooth, it can cause extreme pain that can only be rectified through root canal therapy. Certain risk factors, such as recent procedures, cracks in the teeth and large fillings, can be contributors of disease growing within a tooth. That disease can cause an infection in the tooth pulp, which will necessitate a root canal treatment. Any damage to the teeth, such as a crack or a chip caused by an injury, may also need root canal therapy to fix the damaged area. Tooth pain is a major sign of infection and should not be ignored, but feeling pain is not the only symptom of an infected tooth. Pain while eating or putting pressure on a tooth are common symptoms, but lingering and lasting sensitivity to hot and cold stimuli is a warning sign that something is wrong. Tenderness and swelling of the gums near a tooth can mean an infection, but also if your tooth has taken on a darker shade, make sure to schedule an appointment with your dentist as soon as possible. Occasionally, a small, pimple-like bump might appear on the gums near where the pain is radiating, and that is a sign of infection, as well. Swelling around the face and/or neck, or even a hole in the tooth, are additional signs that your tooth may be infected.
Procedure and Treatment
A root canal is a multi-step dental procedure that focuses on removing the infected tooth pulp and sealing the tooth up again to avoid any future infection or pain. A root canal is usually done by an endodontist or general dentist, and takes one to two visits to complete. First, they will take X-rays of your teeth to see how extensive the damage is and which teeth are affected. Your mouth will then be numbed with a local anesthetic to prevent any pain during the procedure, and a sheet of rubber, called a “rubber dam,” will be placed around the tooth to keep it dry. Next, the dentist or endodontist will drill an access hole into the tooth to remove the damaged nerve and pulp tissue. After cleaning out and drying the tooth, he or she will seal the tooth by filling the root canal with a rubber compound and placing a filling over the hole to cover the access point. Sometimes, the tooth will be left open to drain for several days and medicine put into the pulp chamber to clear out any infection. If the tooth cannot be sealed the same day, your dentist will put in a temporary filling to protect you from any pain until your customized crown is ready. After your crown, filling, or other tooth restoration is fitted, the root canal treatment is finished until you have other follow-up appointments to make any minor adjustments, if needed.
What To Expect After Your Root Canal
Most patients who receive a root canal treatment feel almost instant relief once the infection is removed and the tooth is cleaned out. For those who are sore or have lingering pain, over-the-counter pain medication is normally all one needs to lessen the discomfort. If you have lingering pain that doesn’t dissipate after a few days, make sure to talk with your dentist or endodontist for further evaluation. If you are still waiting to receive your crown or permanent filling, avoid chewing and biting on the treated tooth so as to avoid any additional damage to the healing tooth. Brush and floss your teeth like normal each day, and rinse your mouth with warm salt water to relieve any inflammation. If you stick to a good oral health regimen, your restored tooth can last for a lifetime.